Fever of Unknown Origin: How to Care for Your Child
Fever of unknown origin is when a child has fever for longer than a week and testing doesn't find the cause. The health care team examined your child and did tests, but they found no serious cause of the fever. Your child might have gotten fluids if dehydrated. Your child can be cared for at home. The team will continue checking for test results. Sometimes, test results that show what caused the fever come back after a patient leaves the hospital. Some fevers end without a cause ever being found. Continue to keep track of fever and other symptoms at home.

-
If your child feels warm, take your child's temperature as instructed.
-
Do not use a glass thermometer with mercury because these are not safe.
-
There are different methods available for checking temperature based on a child's age:
-
Babies younger than 3 months: Rectal method is best (in child's bottom).
-
Babies 3–6 months: Rectal method is best. Temporal artery (swiped over forehead) or axillary method (under armpit) also may be used.
-
Kids 6 months–4 years: Rectal method is best. Ear, temporal artery, or axillary method also may be used.
-
Kids 4 years or older: Oral method (under the tongue) is best if the child can properly hold the thermometer under the tongue. If not, rectal, temporal, ear, or axillary method may be used.
-
Axillary and temporal artery methods can be used at any age (including younger than 3 months) to "screen" for fever (get an idea about whether there may be a fever). If these show a fever, double-check by taking a rectal or oral temperature.
-
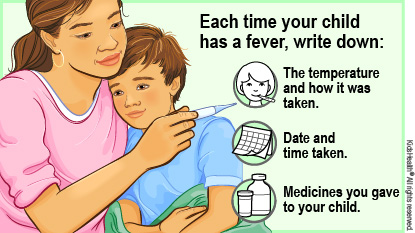
Keep a record of your child's fevers, including:
-
The temperature and how it was taken (such as in the mouth, in the bottom, or under the armpit).
-
The date and time you took the temperature.
-
Any other symptoms your child had at the time (such as headache or belly pain).
-
Any medicines you gave to your child.
-
If your child has a fever and is uncomfortable, a medicine may help your child feel better:
-
If your child has an ongoing medical problem (for example, a kidney, liver, or blood problem): Check with your health care provider before giving any pain or fever medicines.
-
For children under 3 months: Check with your health care provider before giving any pain or fever medicines.
-
For children 3–6 months: You may give acetaminophen (such as Tylenol® or a store brand).
-
For children over 6 months: You may give acetaminophen (such as Tylenol® or a store brand) OR ibuprofen (such as Advil®, Motrin®, or a store brand).
-
Do not give aspirin to your child as it is linked to a rare but serious illness called Reye syndrome.
-
Offer your child plenty of fluids to drink.
-
Let your child rest as needed.
-
Keep any follow-up appointments as recommended. Sometimes, more checkups and testing are done to help find the cause of the fevers.
-
Follow instructions about when your child can return to child care or school.

Your child:
-
develops a new symptom, such as vomiting, diarrhea, cough, rash, bad-smelling pee or pain when peeing (urinating), or pain somewhere in the body (such as belly pain, ear pain, or sore throat)
-
seems to be getting sicker
-
develops a fever again after having no fever for a while
Your child:
-
is very upset and can't be calmed down
-
is hard to wake up
-
appears dehydrated; signs include drowsiness, a dry or sticky mouth, sunken eyes, crying with few or no tears, or peeing less often (or having fewer wet diapers)
-
develops bruising or tiny red dots on the skin
-
has trouble breathing or swallowing
-
has a seizure (body movements that look uncontrolled)

What causes fever? Fever in a child is often due to a viral infection (such as a cold or a stomach bug). Bacterial infections also can cause a fever. When fever comes and goes for a long period of time, health care providers look for rarer non-infectious causes. It can take a while to figure out the cause of the fever. Sometimes the fever ends with no cause found at all.
If my child feels warm, is it always fever? Not all kids who feel warm have a fever. Kids can feel warm when they are very active, play outdoors in hot weather, sleep in warm pajamas under blankets, or are upset and crying. These things make the skin feel hot because the skin is doing its job of getting rid of heat in the body. So, it's best to use a thermometer to measure a temperature if you have any concerns.
What temperature is considered a fever? Temperature taken in different ways can give different readings. These numbers are considered a fever for the type of measurement you take:
|
Type of measurement
|
Where temperature is taken
|
When is the temperature a fever?
|
|
Rectal
|
Bottom
|
100.4°F (38.0°C)
|
|
Temporal Artery
|
Forehead
|
100.4°F (38.0°C)
|
|
Ear
|
Ear
|
100.4°F (38.0°C)
|
|
Oral
|
Mouth
|
100°F (37.8°C)
|
|
Axillary
|
Under armpit
|
99°F (37.2°C)
|
Do all fevers need treatment? No. If your child has a fever but seems well, is alert, is drinking, and is acting normally, there's no need to give medicine. But medicine can be helpful if your child is uncomfortable and not drinking well. Bringing the fever closer to a normal temperature could make your child feel like drinking, which might prevent dehydration.